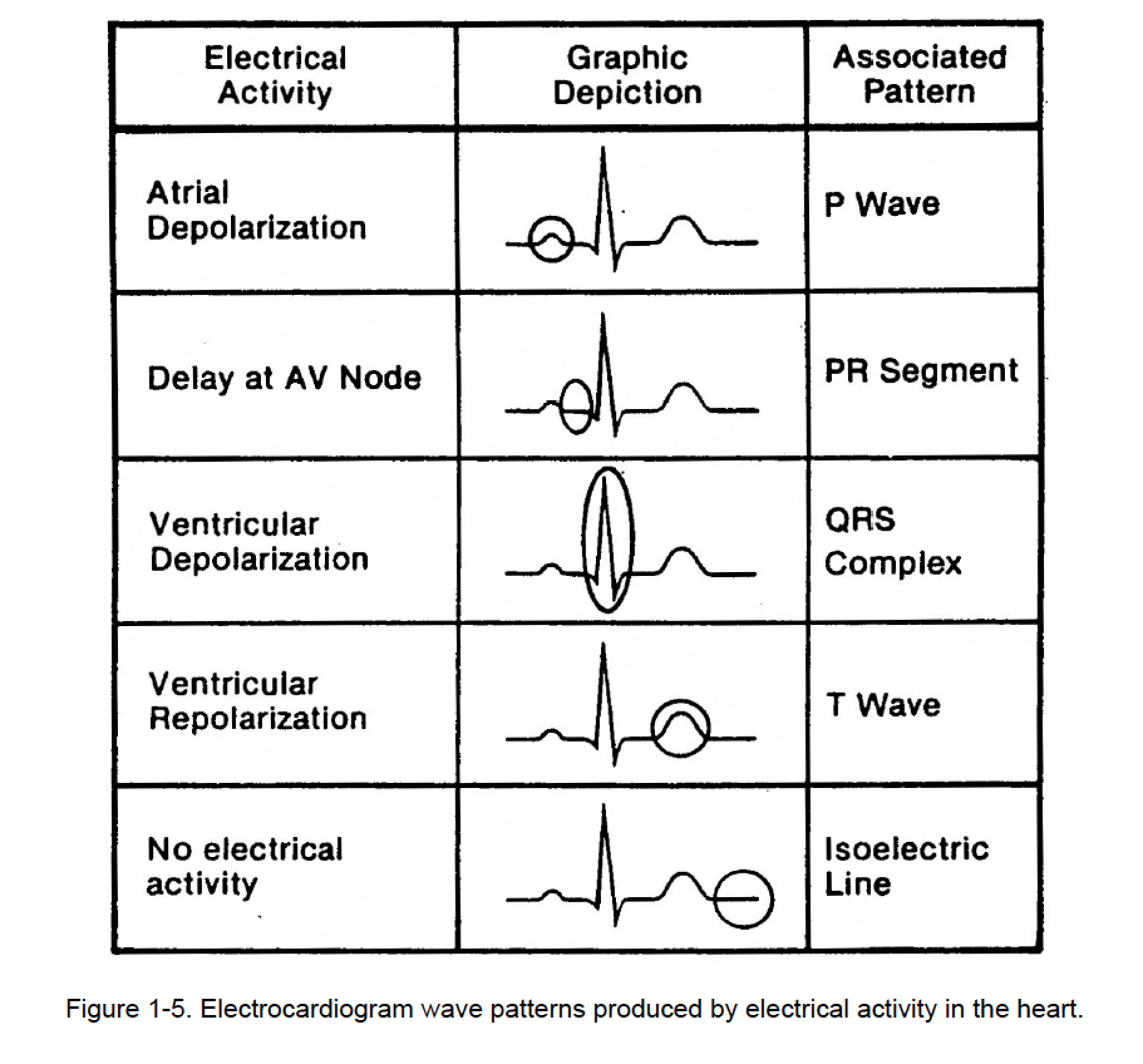
Acquired etiologies that may lead to the development of polymorphic ventricular tachycardia also include drug toxicity of antiarrhythmic drugs, antibiotics, and antipsychotic medications that prolong the QT interval. Congenital conditions predisposing to polymorphic ventricular tachycardia usually exhibit prolongation of the QT interval on the EKG. In polymorphic ventricular tachycardia, the QRS complexes vary in morphology and usually result from inherent genetic mutations that disrupt the ion channel function of cardiac myocytes and cause electrophysiological abnormalities during ventricular repolarization. The most common cause for monomorphic ventricular tachycardia is scarring of the myocardium from myocardial infarction, which promotes the development of an electrical circuit around the non-conducting fibrotic tissue resulting in the formation of multiple circuits that potentially can evolve into a re-entrant ventricular tachyarrhythmia. In monomorphic ventricular tachycardia, which is more common, the QRS complexes are identical because there is increased automaticity originating from a single focus in either of the ventricles or a re-entry circuit within the ventricle. In pulseless ventricular tachycardia, the ventricles contract at a rate too rapid to allow for an adequate filling time during diastole, subsequently resulting in hemodynamic collapse from a diminished cardiac output causing insufficient blood supply to end organs. Abnormal ventricular conduction and asynchrony further reduce the effectiveness of ventricular contractions and aggravate the hemodynamics, leading to sudden collapse. There are two main types of ventricular tachycardia with the morphology of the QRS complexes serving as clues to the cause responsible for the rhythm. Electrical impulses originating in ventricular myocardium spread through ischemic myocardium or scar tissue resulting in retrograde atria activation or AV dissociation. Įlectrophysiological mechanisms of pulseless ventricular tachycardia are increased automaticity and triggered activity. The most common cause of pulseless ventricular tachycardia is cardiac ischemia. The ventricular arrhythmia can be characterized as either monomorphic (no variation of the QRS from beat to beat) or polymorphic (changing or multiform QRS from beat to beat). There are several scoring systems to differentiate ventricular tachycardia from a wide complex supraventricular tachycardia, but 90% of wide complex tachycardia cases will be ventricular tachycardia. 
Electrophysiology identifying factors for pulseless ventricular tachycardia include tachycardia (>100 bpm), wide QRS complexes (> 120 milliseconds), atrioventricular (AV) dissociation, presence of fusion or capture beats and an electrical axis between -90 to -180. 
Pulseless ventricular tachycardia is a medical emergency.ĭue to rapid ventricular contractions, the ventricular filling decreases markedly, leading to a dramatic decrease in cardiac output. Pulseless ventricular tachycardia is a life-threatening cardiac arrhythmia in which coordinated ventricular contractions are replaced by very rapid but ineffective contractions, leading to insufficient organ perfusion and heart failure.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
